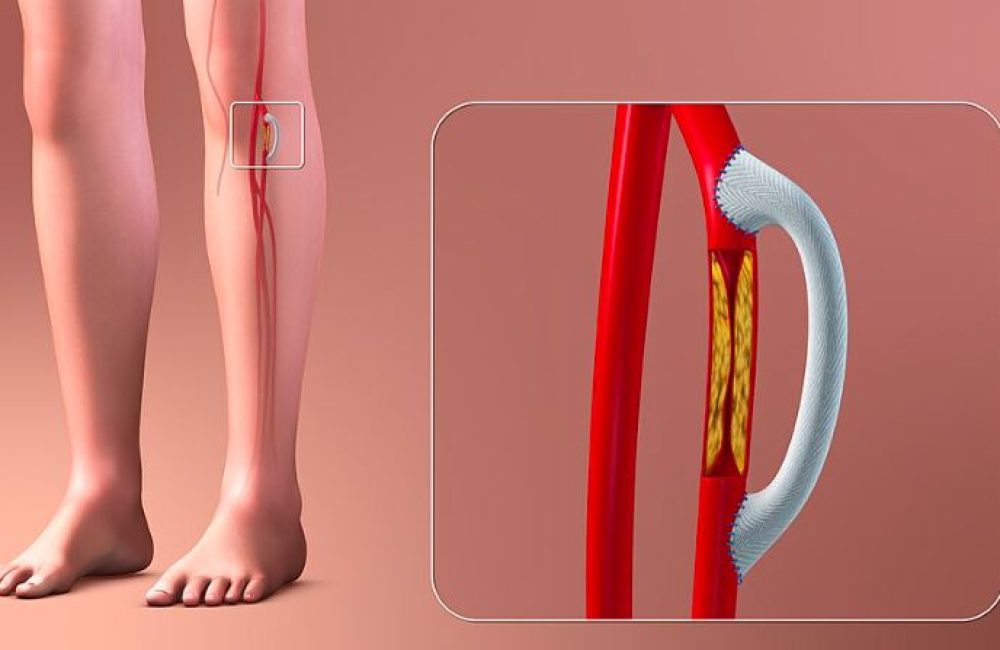
Vascular bypass is a surgical procedure used to restore adequate blood flow to an area of the body when an artery is blocked or severely narrowed. The operation involves creating an alternate route, or “bypass,” around the diseased section of the blood vessel using either a vein from the patient’s body or a synthetic graft. Vascular bypass is a critical intervention for patients with peripheral arterial disease (PAD), severe limb ischemia, or other vascular conditions that threaten the viability of limbs or organs. By improving circulation, it helps relieve pain, prevent tissue damage, and in many cases, saves the limb from amputation.
Arteries are the blood vessels responsible for carrying oxygen-rich blood from the heart to tissues throughout the body. In conditions such as atherosclerosis, fatty deposits (plaques) accumulate inside the arteries, narrowing or blocking them. When this occurs in the arteries supplying the legs, it can lead to critical limb ischemia—a severe reduction in blood supply that causes pain, ulcers, or even gangrene.
A vascular bypass reroutes the blood around the obstruction, ensuring tissues downstream continue to receive oxygen and nutrients. Depending on the site of blockage, bypasses can be performed in the aorta, femoral arteries, popliteal arteries, or smaller arteries of the lower leg.
The main underlying cause of arterial blockages requiring bypass surgery is atherosclerosis, which develops from the gradual buildup of fatty deposits in the arterial walls. Risk factors include:
Smoking – the most significant risk factor for vascular disease.
Diabetes mellitus – accelerates vascular damage and increases risk of infection.
High blood pressure (hypertension) – damages arterial walls over time.
High cholesterol levels – contribute to plaque buildup.
Obesity and sedentary lifestyle – increase vascular strain.
Family history of vascular disease – genetic predisposition.
Age – older adults are at higher risk.
Other causes include arterial injury, inflammation (vasculitis), or congenital vascular abnormalities.
Patients requiring vascular bypass often present with:
Claudication – cramping or pain in the legs during walking, relieved by rest.
Rest pain – severe pain in the feet or toes, worse at night.
Non-healing wounds or ulcers – particularly on the toes or lower legs.
Skin changes – coolness, discoloration, or thinning of the skin.
Gangrene – tissue death due to lack of blood supply.
Symptoms can range from mild discomfort to life-threatening tissue loss.
Diagnosis involves a combination of clinical examination and diagnostic testing:
Medical history and physical exam – checking pulses in the legs, skin color, and temperature.
Ankle-Brachial Index (ABI) – a simple test comparing blood pressure in the ankle with that in the arm to assess circulation.
Doppler ultrasound – evaluates blood flow and identifies areas of narrowing.
CT angiography or MR angiography – provides detailed imaging of arteries.
Conventional angiography – an invasive test in which dye is injected to visualize blood flow, often performed when surgical intervention is planned.
Before surgery, patients are often managed with conservative measures:
Lifestyle modification – quitting smoking, regular exercise, weight management.
Medications – antiplatelet drugs (aspirin, clopidogrel), cholesterol-lowering agents (statins), blood pressure control, and diabetes management.
Supervised exercise therapy – improves walking distance and circulation.
If symptoms persist or if there is critical limb ischemia, surgical options include:
Endovascular interventions – angioplasty, stenting, or atherectomy to reopen narrowed arteries.
Vascular bypass surgery – performed when blockages are too extensive or unsuitable for endovascular treatment.
Vascular bypass surgery typically involves the following steps:
Anesthesia – general or regional anesthesia is administered.
Incision – the surgeon makes incisions above and below the blockage.
Graft selection – a vein (often the saphenous vein from the leg) or a synthetic graft is prepared.
Bypass creation – the graft is attached to the artery above and below the obstruction, forming a new pathway for blood flow.
Closure – the surgical site is carefully closed, and circulation through the bypass is checked.
The length and complexity of the procedure depend on the site and extent of disease.
Recovery involves close monitoring in the hospital and long-term follow-up:
Hospital stay – usually 3–7 days depending on recovery.
Wound care – keeping surgical sites clean and monitoring for infection.
Medications – continued use of antiplatelet drugs and statins to prevent clotting or graft failure.
Lifestyle changes – smoking cessation, exercise programs, and healthy diet.
Physical therapy – gradual return to walking and activity.
Regular follow-up – monitoring graft patency with ultrasound and clinical exams.
As with any major surgery, vascular bypass carries risks, including:
Infection at the incision site or graft.
Blood clots within the bypass graft.
Bleeding or hematoma formation.
Graft failure or narrowing over time.
Heart attack, stroke, or other cardiovascular events (especially in patients with widespread atherosclerosis).
Limb swelling or nerve injury near the incision site.
Seek medical attention if you experience:
Persistent leg pain or cramping while walking.
Severe foot pain, especially at rest.
Non-healing sores or ulcers on the legs or feet.
Changes in skin color, temperature, or loss of hair on the legs.
Signs of infection or sudden worsening of symptoms after vascular surgery.
Prompt medical evaluation can prevent complications and improve outcomes.
Vascular bypass is a vital surgical option for patients with severe arterial blockages, particularly in the legs. By rerouting blood flow around diseased arteries, it restores circulation, relieves pain, and saves limbs at risk. Although the procedure carries risks, the benefits are substantial when combined with lifestyle changes, medical therapy, and regular follow-up. Anyone experiencing symptoms of poor circulation should seek timely medical advice to explore appropriate treatment options and protect long-term vascular health.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec