Thoracic Endovascular Aneurysm Repair (TEVAR) is a minimally invasive surgical procedure used to treat aneurysms of the thoracic aorta — the major blood vessel that carries blood from the heart through the chest. A thoracic aortic aneurysm (TAA) is a dangerous condition characterized by a localized dilation or bulging of the aorta wall, which can lead to life-threatening rupture if left untreated. TEVAR has revolutionized the management of thoracic aortic aneurysms by offering a less invasive alternative to open surgery, reducing recovery time, and improving patient outcomes. This article provides a detailed, reader-friendly guide to TEVAR, covering its background, indications, procedure, and more.
The aorta is the largest artery in the body, originating from the left ventricle of the heart and extending through the chest (thoracic aorta) and abdomen (abdominal aorta). The thoracic aorta is divided into several segments: the ascending aorta, the aortic arch, and the descending thoracic aorta. It supplies oxygen-rich blood to the head, neck, arms, and upper body.
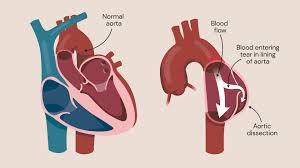
An aneurysm occurs when a section of the aortic wall weakens and balloons outward. In the thoracic region, aneurysms can affect any part of the aorta but are most commonly found in the descending thoracic aorta. The risk of rupture increases with the size of the aneurysm, making timely diagnosis and treatment critical.
Several factors contribute to the development of thoracic aortic aneurysms, including:
Thoracic aortic aneurysms often grow silently and may remain asymptomatic until they reach a significant size or rupture. When symptoms occur, they may include:
Diagnosis of thoracic aortic aneurysm involves a combination of clinical evaluation and imaging studies:
While TEVAR is generally safer than open surgery, potential risks include:
TEVAR has significantly improved the prognosis for patients with thoracic aortic aneurysms, offering lower perioperative morbidity and mortality compared to open repair. Long-term outcomes depend on aneurysm size, patient comorbidities, and adherence to follow-up. Regular surveillance is essential to detect complications early.
Seek immediate medical attention if you experience:
Early consultation with a vascular surgeon or cardiologist is recommended if you have risk factors or a family history of aneurysms.
horacic Endovascular Aneurysm Repair (TEVAR) represents a major advancement in the treatment of thoracic aortic aneurysms, offering a less invasive option with improved recovery and outcomes. Understanding the anatomy, risk factors, symptoms, and treatment options is crucial for timely diagnosis and management. If you or a loved one is diagnosed with a thoracic aortic aneurysm, consult a healthcare professional to discuss the best individualized treatment plan. Early intervention can save lives and improve quality of life.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec