Femoro-popliteal (fem-pop) bypass is a surgical procedure performed to restore blood flow in the thigh and leg when the femoral or popliteal arteries are severely narrowed or blocked. These arteries are critical for supplying blood to the lower limbs, and when circulation is compromised, it can cause pain, ulcers, or even threaten the viability of the leg. The surgery involves rerouting blood around the blocked section of the artery using a graft, which may be a vein from the patient’s own body or a synthetic tube.
This operation is most often performed in people with peripheral arterial disease (PAD) and plays a crucial role in preventing limb loss, improving walking ability, and relieving pain.
The femoral artery runs along the thigh, carrying oxygen-rich blood from the aorta into the lower limb. As it travels down the leg, it passes through the thigh and knee region, where it becomes the popliteal artery, located behind the knee. From there, the popliteal artery branches into smaller vessels that continue into the lower leg and foot.
Blockage in the femoral or popliteal artery interrupts this blood flow, particularly affecting the muscles and tissues of the lower leg and foot. A femoro-popliteal bypass restores circulation by creating a new channel that bridges the obstruction.
The most common cause requiring a fem-pop bypass is atherosclerosis—a buildup of fatty deposits and calcium (plaque) inside the arterial wall. Over time, this leads to hardening and narrowing of the arteries. Key risk factors include:
Smoking – the single most significant risk factor.
Diabetes mellitus – damages blood vessels and increases the risk of infection.
High cholesterol levels – accelerate plaque buildup.
Hypertension (high blood pressure) – damages artery walls.
Obesity and sedentary lifestyle – contribute to vascular disease progression.
Older age – risk increases with advancing age.
Family history of vascular disease – genetic predisposition.
Less common causes include trauma, arterial inflammation, or blood clot disorders.
When blood flow through the femoral or popliteal artery is reduced, patients may experience:
Intermittent claudication – pain or cramping in the calf or thigh during walking that eases with rest.
Rest pain – severe foot or toe pain, particularly at night.
Non-healing wounds or ulcers – often on the toes, feet, or ankles.
Coolness, numbness, or weakness – in the affected leg.
Skin changes – pale, bluish, or shiny skin on the lower leg.
Gangrene – in severe cases, tissue death due to lack of oxygen.
These symptoms can significantly reduce quality of life and, if untreated, may lead to amputation.
Diagnosis begins with a detailed clinical assessment and is confirmed with vascular imaging. Common steps include:
History and physical examination – including pulse checks in the legs and assessment of wounds.
Ankle-Brachial Index (ABI) – compares blood pressure at the ankle and arm to detect reduced circulation.
Doppler ultrasound – evaluates blood flow and identifies blockages.
CT angiography or MR angiography – provides detailed 3D images of the arteries.
Conventional angiography – dye is injected into the arteries for a precise view, often done before surgical planning.
For many patients, symptoms can be managed initially with:
Lifestyle modification – smoking cessation, regular exercise, healthy diet.
Medications – antiplatelet drugs (aspirin, clopidogrel), cholesterol-lowering statins, and medicines for diabetes and hypertension.
Exercise therapy – supervised walking programs improve circulation and endurance.
When symptoms are severe or tissue loss is imminent, invasive procedures are considered:
Endovascular treatments – such as angioplasty (inflating a balloon to widen the artery) and stenting (placing a metal scaffold to keep the artery open).
Femoro-popliteal bypass surgery – performed when blockages are long, severe, or unsuitable for endovascular treatment.
A femoro-popliteal bypass involves several steps:
Anesthesia – general or regional anesthesia is administered.
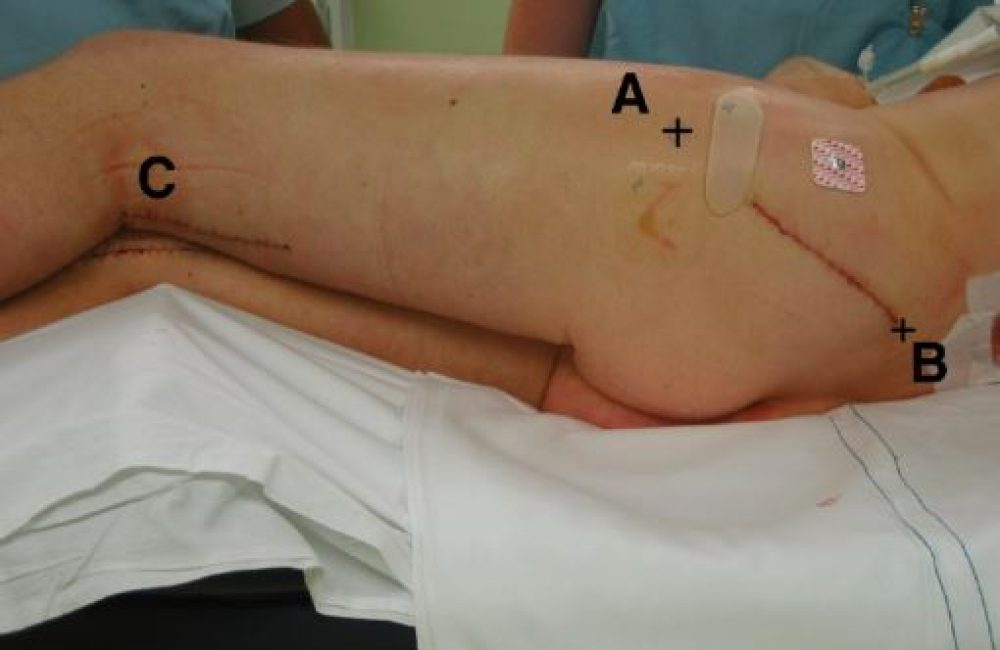
Incisions – made in the groin (near the femoral artery) and behind the knee (near the popliteal artery).
Graft preparation – the surgeon selects a graft, either the patient’s saphenous vein (preferred for durability) or a synthetic graft if a vein is not available.
Bypass creation – the graft is sewn into the femoral artery above the blockage and into the popliteal artery below the blockage, creating a new route for blood flow.
Closure – the surgical wounds are closed, and blood flow through the graft is checked.
The surgery usually takes 2–4 hours, depending on complexity.
Recovery requires careful hospital monitoring and long-term follow-up:
Hospital stay – typically 4–7 days.
Pain management and wound care – to promote healing and prevent infection.
Antiplatelet therapy – to reduce the risk of clotting in the graft.
Early mobilization – walking is encouraged soon after surgery to stimulate circulation.
Lifestyle modifications – quitting smoking, controlling diabetes, and maintaining a healthy weight are critical.
Follow-up imaging – Doppler ultrasound is used periodically to ensure the graft remains open.
As with any major vascular surgery, risks include:
Infection – particularly at the graft or incision site.
Bleeding or hematoma – at surgical sites.
Graft failure or thrombosis – blockage of the bypass.
Cardiac complications – such as heart attack or arrhythmia in patients with cardiovascular disease.
Limb swelling or nerve injury – temporary or permanent.
Wound healing issues – more common in diabetic or frail patients.
Medical attention should be sought if you experience:
Persistent leg pain or cramping with activity.
Severe foot pain at rest.
Non-healing wounds or ulcers on the lower limb.
Sudden changes in skin color, temperature, or sensation in the leg.
Signs of infection or worsening symptoms after bypass surgery.
Early detection and timely treatment improve the chances of successful outcomes.
Femoro-popliteal bypass is a vital surgical procedure for patients with advanced peripheral arterial disease and severe leg artery blockages. By rerouting blood around diseased arteries, it restores circulation, relieves pain, and can prevent limb loss. While the operation carries some risks, its benefits are significant, especially when combined with lifestyle changes, medications, and long-term follow-up.
Anyone experiencing symptoms of poor circulation—such as pain, ulcers, or changes in skin color of the legs—should consult a healthcare professional promptly to explore treatment options and protect their vascular health.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec