An Aorto-Bifemoral Bypass is a major vascular surgery performed to restore blood flow to the legs when the aorta and iliac arteries are severely narrowed or blocked. These vessels supply oxygen-rich blood to the pelvis and lower limbs. When blockages occur, patients may develop pain, disability, or life-threatening complications such as limb ischemia.
The surgery involves creating a bypass from the abdominal aorta (the body’s main artery) to both femoral arteries in the groin using a synthetic graft. It is considered the gold standard treatment for extensive aortoiliac occlusive disease when less invasive options are not suitable. By re-establishing circulation, the procedure relieves pain, improves walking ability, and prevents limb loss.
The abdominal aorta is the largest artery in the body, carrying blood from the heart through the abdomen. It branches into the common iliac arteries, which then divide into external and internal iliac arteries. The external iliac arteries continue into the thighs as the femoral arteries, delivering blood to the legs.
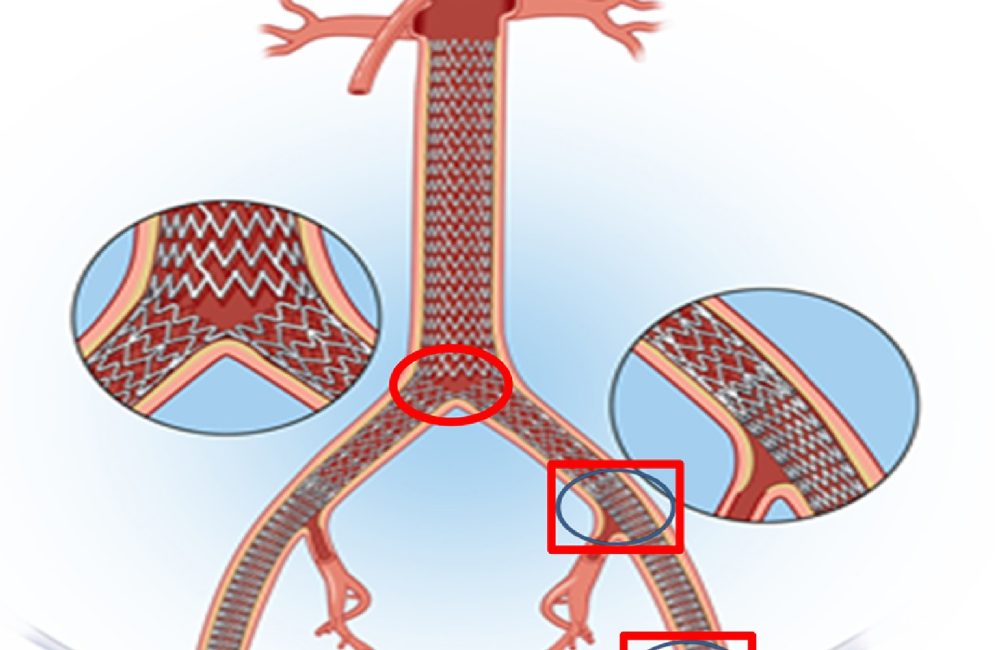
When these arteries are blocked by plaque buildup (atherosclerosis), blood flow to both legs can be critically reduced. An aorto-bifemoral bypass creates a new path by sewing a Y-shaped graft to the aorta above the diseased section and connecting the limbs of the graft to the femoral arteries in the groin.
The main cause of blockages requiring an aorto-bifemoral bypass is atherosclerosis, a condition where fatty deposits, calcium, and scar tissue build up inside arteries, narrowing or obstructing them.
Key risk factors include:
Smoking – the strongest preventable risk factor.
Diabetes mellitus – accelerates arterial disease and impairs healing.
High cholesterol levels – contribute to plaque formation.
Hypertension (high blood pressure) – damages artery walls over time.
Obesity and inactivity – increase cardiovascular strain.
Advancing age – arteries naturally stiffen and become more prone to disease.
Family history of vascular disease – genetic predisposition.
Rarely, arterial blockages may also result from trauma, blood clots, or inflammatory conditions affecting blood vessels.
Patients with severe aortoiliac blockages may present with:
Claudication – cramping pain in the buttocks, thighs, or calves while walking, relieved by rest.
Rest pain – severe pain in the feet, especially at night.
Coldness or numbness – in the legs or feet.
Skin changes – pale, bluish, or thin shiny skin.
Non-healing wounds or ulcers – particularly on the feet or toes.
Impotence in men – sometimes associated with aortoiliac disease (Leriche’s syndrome).
Gangrene – tissue death in severe cases.
Symptoms usually worsen gradually but can sometimes progress quickly if a clot suddenly blocks the artery.
A thorough clinical and imaging evaluation is essential for diagnosis and surgical planning:
History and physical exam – assessing walking distance, leg pain, and palpating pulses in the groin and legs.
Ankle-Brachial Index (ABI) – compares blood pressure in the ankle and arm to detect circulation problems.
Doppler ultrasound – evaluates blood flow and identifies narrowed or blocked segments.
CT angiography or MR angiography – provides detailed images of the aorta and iliac arteries.
Conventional angiography – performed in select cases for precise mapping before intervention.
In early or mild cases, treatment may focus on:
Lifestyle changes – quitting smoking, diet improvement, and regular exercise.
Medications – antiplatelet agents (aspirin, clopidogrel), cholesterol-lowering statins, and drugs to control diabetes and hypertension.
Supervised exercise therapy – improves walking distance and stimulates collateral circulation.
When symptoms are severe or tissue is at risk:
Endovascular therapy – angioplasty and stenting may be performed for less extensive disease.
Aorto-bifemoral bypass surgery – considered when blockages are long, severe, or unsuitable for endovascular treatment.
Aorto-bifemoral bypass is performed under general anesthesia. The main steps include:
Abdominal incision – to access the abdominal aorta above the blockage.
Groin incisions – to expose both femoral arteries.
Graft selection – a synthetic Y-shaped graft (usually made of Dacron or PTFE) is prepared.
Bypass creation – the top of the graft is sewn into the aorta above the blockage, while each limb of the graft is sewn into the femoral arteries in the groin.
Circulation check – blood flow through the graft is confirmed.
Closure – incisions are closed carefully, and drains may be placed.
The surgery usually takes 4–6 hours, depending on complexity.
After surgery, patients are monitored closely in the hospital, often in an intensive care setting initially.
Hospital stay – usually 7–10 days.
Pain and wound care – incisions in the abdomen and groins require careful monitoring.
Mobility – walking is encouraged early to promote circulation.
Medications – lifelong antiplatelet therapy and statins to prevent graft clotting.
Lifestyle adjustments – quitting smoking, exercise, and weight management are critical for long-term success.
Follow-up imaging – Doppler ultrasound and CT scans may be performed to monitor graft function.
Aorto-bifemoral bypass is a major surgery and carries certain risks, including:
Infection of the graft or surgical wounds.
Bleeding or hematoma formation.
Graft thrombosis (blockage of the bypass).
Heart attack, stroke, or lung complications.
Kidney problems due to reduced blood flow during surgery.
Bowel complications (rare but serious).
Lymphatic fluid leaks or leg swelling.
While risks exist, advances in surgical techniques and perioperative care have greatly improved safety.
The procedure has excellent long-term outcomes, particularly when risk factors are managed.
Patency rates (graft openness) are high: many grafts remain functional for 10 years or more.
Most patients experience significant symptom relief and improved walking ability.
Limb salvage rates are excellent when surgery is performed before advanced tissue loss.
Long-term success depends heavily on lifestyle changes, especially smoking cessation and control of diabetes and cholesterol.
Prompt medical evaluation is necessary if you experience:
Persistent pain in the legs or buttocks with walking.
Severe foot pain at rest, especially at night.
Non-healing ulcers or blackened toes/feet.
Sudden worsening of symptoms, including loss of pulses in the legs.
Signs of infection, swelling, or drainage after bypass surgery.
Early intervention improves outcomes and may prevent limb-threatening complications.
Aorto-bifemoral bypass is a vital surgical treatment for advanced aortoiliac occlusive disease. By creating a new pathway for blood to flow from the aorta to both femoral arteries, it restores circulation, relieves pain, and helps preserve limb function. Though it is a major operation with risks, the long-term results are excellent when paired with healthy lifestyle changes and consistent follow-up care.
Anyone experiencing persistent leg pain, walking difficulties, or non-healing wounds should seek medical advice promptly. Early diagnosis and appropriate treatment can make the difference between restoring mobility and facing serious complications such as limb loss.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec