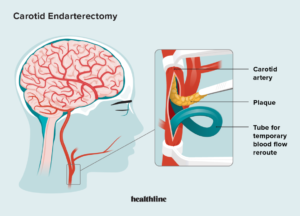
Carotid endarterectomy (CEA) is a surgical procedure aimed at preventing stroke by removing atherosclerotic plaque from the carotid artery. The carotid arteries are major blood vessels in the neck that supply oxygen-rich blood to the brain. When these arteries become narrowed or blocked due to plaque buildup, the risk of ischemic stroke increases significantly. CEA is an important intervention for patients with significant carotid artery stenosis, especially those who have experienced transient ischemic attacks (TIAs) or minor strokes. This article provides a detailed, reader-friendly overview of carotid endarterectomy, including its background, indications, procedure, and postoperative care.
The carotid arteries are paired vessels located on each side of the neck. Each artery branches into the internal and external carotid arteries. The internal carotid artery supplies blood to the brain, while the external carotid artery supplies the face and scalp. The common carotid artery bifurcates into these two branches at approximately the level of the thyroid cartilage.
Atherosclerosis, the buildup of fatty plaques within the arterial walls, can cause narrowing (stenosis) of the internal carotid artery. This narrowing reduces blood flow to the brain and can lead to the formation of blood clots that may travel to the brain, causing a stroke. Carotid endarterectomy involves surgically removing these plaques to restore normal blood flow and reduce stroke risk.
The primary cause of carotid artery stenosis is atherosclerosis, a chronic inflammatory condition characterized by the accumulation of lipids, cholesterol, calcium, and cellular debris within the arterial walls. Several risk factors contribute to the development of atherosclerosis and carotid artery disease:
Carotid artery stenosis may be asymptomatic initially. When symptoms occur, they often result from reduced cerebral blood flow or embolization of plaque fragments. Common clinical presentations include:
Diagnosis of carotid artery stenosis involves a combination of clinical evaluation and imaging studies:
Clinical Examination:
Imaging Investigations:
The degree of stenosis is typically quantified as a percentage narrowing of the arterial lumen, which guides treatment decisions.
Treatment depends on the size, location, symptoms, and risk of complications.
Carotid endarterectomy is performed under general or regional anesthesia. The key steps include:
Intraoperative monitoring of cerebral perfusion may be performed using EEG or cerebral oximetry to ensure adequate brain blood flow during clamping.
Most patients recover within days to weeks, with gradual return to normal activities.
While carotid endarterectomy is generally safe, potential risks include:
Carotid endarterectomy significantly reduces the risk of stroke in appropriately selected patients. The procedure has a high success rate, with most patients experiencing improved cerebral blood flow and symptom relief. Long-term outcomes depend on control of cardiovascular risk factors and adherence to medical therapy. Regular follow-up is essential to monitor for restenosis.
Seek medical attention promptly if you experience:
Early evaluation can lead to timely diagnosis and prevention of stroke.
Carotid endarterectomy is a vital surgical procedure for preventing stroke in patients with significant carotid artery stenosis. Understanding the anatomy, causes, symptoms, and treatment options helps patients and caregivers make informed decisions. While the surgery carries some risks, its benefits in reducing stroke risk are well established. If you or a loved one experience symptoms suggestive of carotid artery disease, consult a healthcare professional promptly for evaluation and management. Early intervention can save lives and improve quality of life.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec