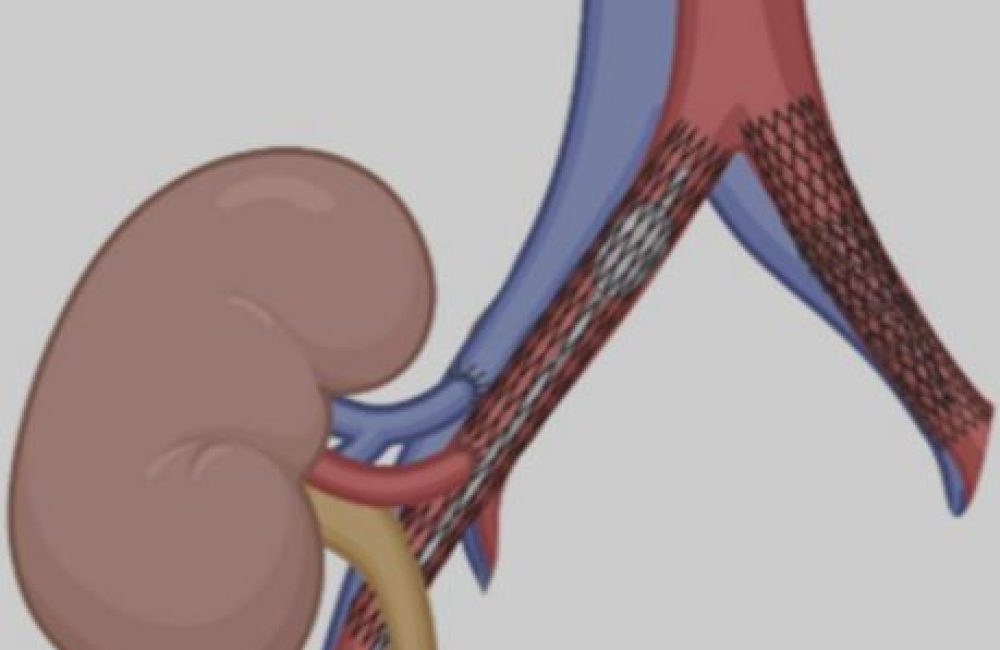
Iliac angioplasty is a minimally invasive procedure used to treat blockages or narrowing of the common iliac artery (CIA) or external iliac artery (EIA). These arteries are major blood vessels in the pelvis that supply blood to the legs. When narrowed due to atherosclerosis or other vascular disease, blood flow to the lower limbs becomes restricted, causing pain, walking difficulties, and in severe cases, limb-threatening ischemia. Iliac angioplasty restores circulation, improves mobility, and helps prevent complications such as ulcers, gangrene, and amputation.
The aorta, the body’s main artery, divides into the right and left common iliac arteries in the lower abdomen. Each common iliac artery then branches into the internal iliac artery, supplying blood to the pelvis, and the external iliac artery, which continues into the thigh as the femoral artery. Together, these arteries provide essential circulation to the legs. When the CIA or EIA becomes narrowed or blocked, it significantly impairs blood flow, often leading to peripheral arterial disease (PAD) symptoms.
The primary cause of iliac artery narrowing is atherosclerosis, a condition in which fatty deposits (plaques) build up on artery walls. Risk factors include:
Smoking – the strongest contributor to PAD and iliac artery disease.
Diabetes mellitus – accelerates plaque formation and impairs healing.
High cholesterol and triglycerides – promote arterial plaque build-up.
Hypertension – damages artery walls over time.
Obesity and sedentary lifestyle – increase cardiovascular risk.
Age and family history – older adults and those with genetic predisposition are more at risk.
Chronic kidney disease – associated with vascular calcification and arterial stiffness.
Iliac artery disease can present with a range of symptoms depending on the severity of narrowing:
Intermittent claudication – cramping or pain in the thighs, buttocks, or calves during walking or exercise, relieved by rest.
Rest pain – continuous pain in the feet or toes, often worse at night.
Non-healing ulcers or sores on the legs or feet.
Coldness, numbness, or discoloration in the affected limb.
Weak or absent pulses in the groin or legs.
Erectile dysfunction in men (especially when combined with claudication, known as Leriche’s syndrome).
Accurate diagnosis is essential to plan treatment. Common diagnostic steps include:
Clinical assessment – checking for reduced or absent pulses, skin changes, and wound healing problems.
Ankle-Brachial Index (ABI) – comparing blood pressure at the ankle with that in the arm; a low ABI suggests arterial disease.
Duplex ultrasound – non-invasive imaging to assess blood flow and detect narrowing.
CT Angiography (CTA) or MR Angiography (MRA) – provides detailed visualization of the iliac arteries.
Digital Subtraction Angiography (DSA) – the gold standard test, often performed just before intervention to confirm the site and severity of disease.
Management of iliac artery disease involves both lifestyle changes and medical or interventional therapies:
Lifestyle modifications – quitting smoking, exercise programs, and healthy eating.
Medications – antiplatelet therapy (aspirin, clopidogrel), cholesterol-lowering drugs (statins), and drugs for diabetes and hypertension control.
Wound care – for patients with ulcers or non-healing wounds.
Iliac angioplasty with or without stenting – first-line treatment for many patients due to high success rates.
Bypass surgery (aorto-femoral or femoro-femoral bypass) – reserved for patients with extensive disease not suitable for angioplasty.
Hybrid procedures – combining open surgery with endovascular techniques in complex cases.
Iliac angioplasty is performed in a catheterization laboratory by a vascular specialist:
Preparation – local anesthesia with sedation is given, and the groin area is cleaned.
Access – a catheter is inserted through a puncture in the femoral artery.
Imaging – angiography is performed using contrast dye and X-rays to identify the blockage.
Balloon angioplasty – a balloon-tipped catheter is advanced to the narrowing and inflated to widen the artery.
Stent placement (if required) – a small metal mesh tube is often deployed to keep the artery open and prevent re-narrowing.
Completion angiography – checks blood flow and confirms a successful result.
Closure – the catheter is removed, and the puncture site is sealed with manual pressure or a closure device.
The procedure typically takes 1–2 hours, and most patients are discharged the same or next day.
Recovery after iliac angioplasty is usually quick, but long-term care is essential:
Hospital monitoring – for bleeding, clotting, or puncture site complications.
Medications – dual antiplatelet therapy (aspirin and clopidogrel) for several months to prevent stent blockage.
Lifestyle changes – quitting smoking, diet modification, and physical activity are vital.
Supervised exercise therapy – improves walking ability and long-term vascular health.
Regular follow-up – duplex ultrasound or ABI testing to monitor stent patency.
Although safe and effective, iliac angioplasty carries some risks:
Bleeding or hematoma at the puncture site.
Allergic reaction to contrast dye.
Arterial dissection or rupture during ballooning.
Restenosis – re-narrowing inside the stent over time.
Blood clot formation within the stent.
Kidney injury from contrast dye in susceptible patients.
Infection (rare).
Iliac angioplasty offers excellent long-term results, with high initial success rates (over 90%) and good durability, especially with stenting. Many patients experience significant improvement in walking ability, healing of ulcers, and overall quality of life. Long-term success depends on strict control of risk factors, adherence to medications, and regular follow-up with a vascular specialist.
Patients should seek medical advice if they notice:
Leg pain during walking that improves with rest.
Persistent pain in the feet or toes, especially at night.
Non-healing wounds or ulcers on the legs.
Changes in skin color, coldness, or numbness in the limb.
Sudden worsening of symptoms, which may indicate acute limb ischemia.
Iliac angioplasty (CIA/EIA) is a modern, minimally invasive treatment that effectively restores blood flow in patients with iliac artery disease. By relieving symptoms, promoting healing, and reducing the risk of limb loss, it provides significant benefits with fewer risks and faster recovery compared to open surgery. Early recognition of symptoms and timely consultation with a vascular specialist are key to ensuring the best outcomes.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec