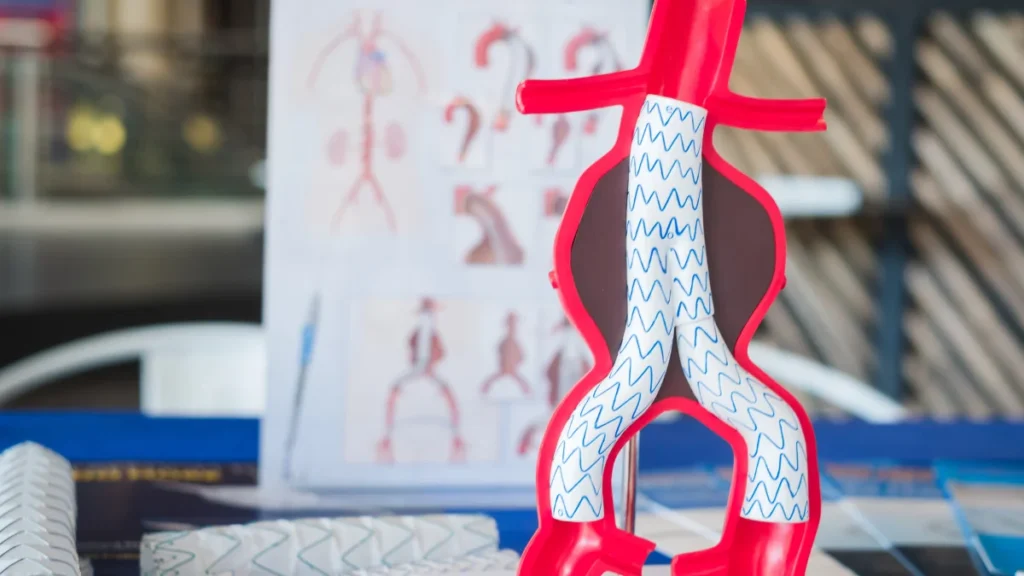
An aortic aneurysm is a dangerous condition characterized by an abnormal bulging or dilation of the aorta, the largest artery in the body. When this dilation occurs in the abdominal section of the aorta, it is called an abdominal aortic aneurysm (AAA). If left untreated, an aneurysm can rupture, leading to life-threatening internal bleeding. Endovascular Aortic Aneurysm Repair (EVAR) is a minimally invasive surgical technique designed to treat AAAs by reinforcing the weakened section of the aorta with a stent graft. EVAR has revolutionized the management of aortic aneurysms by offering a less invasive alternative to open surgery, resulting in reduced recovery times and lower complication rates.
The aorta is the main artery that carries oxygen-rich blood from the heart to the rest of the body. It is divided into several segments: the ascending aorta, the aortic arch, the descending thoracic aorta, and the abdominal aorta. The abdominal aorta extends from the diaphragm to the point where it bifurcates into the iliac arteries supplying blood to the lower limbs.
An aneurysm occurs when the wall of the aorta weakens and balloons outward. The abdominal aorta is particularly susceptible due to its exposure to high blood pressure and the presence of atherosclerotic plaques. The risk of rupture increases as the aneurysm enlarges, making timely diagnosis and treatment critical.
Several factors contribute to the development of an abdominal aortic aneurysm:
Many abdominal aortic aneurysms are asymptomatic and discovered incidentally during imaging for other reasons. When symptoms do occur, they may include:
Diagnosis of an abdominal aortic aneurysm involves a combination of clinical evaluation and imaging studies:
Small aneurysms (typically less than 5.5 cm in diameter) may be managed conservatively with:
Surgical intervention is recommended for:
Two main surgical approaches exist:
EVAR is performed under general or regional anesthesia and involves the following steps:
EVAR avoids the need for a large abdominal incision and aortic cross-clamping, reducing operative stress.
After EVAR, patients typically experience:
Follow-up care includes:
While EVAR is generally safer than open repair, potential risks include:
EVAR has significantly improved the prognosis for patients with abdominal aortic aneurysms. Compared to open repair, EVAR offers:
However, patients must adhere to follow-up schedules to detect and manage late complications.
Seek immediate medical attention if you experience:
For routine screening, men aged 65-75 with a history of smoking should consider abdominal ultrasound to detect aneurysms early.
Endovascular Aortic Aneurysm Repair (EVAR) represents a major advancement in the treatment of abdominal aortic aneurysms, offering a less invasive option with reduced recovery times and improved safety profiles. Understanding the anatomy, risk factors, symptoms, and treatment options is essential for timely diagnosis and management. If you are at risk or have been diagnosed with an aneurysm, consult a vascular specialist to discuss the best treatment approach tailored to your condition. Early intervention and regular follow-up can save lives and improve quality of life.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec