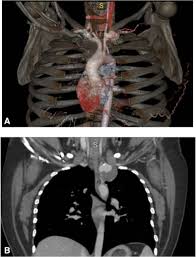
A subclavian artery aneurysm is a rare but potentially serious vascular condition characterized by an abnormal dilation or bulging of the subclavian artery, which supplies blood to the upper limbs, chest, and brain. Although uncommon, these aneurysms are clinically significant due to the risk of rupture, thrombosis, embolization, or compression of adjacent structures such as nerves and veins. Early recognition and appropriate management are crucial to prevent life-threatening complications. This article provides a detailed exploration of subclavian artery aneurysms, covering anatomy, causes, symptoms, diagnosis, treatment options, and prognosis.
The subclavian artery is a major artery that originates from the aortic arch on the left side and from the brachiocephalic trunk on the right side. It travels laterally beneath the clavicle (collarbone) and over the first rib, supplying oxygenated blood to the upper extremities, parts of the thorax, neck, and brain via its branches.
The artery is divided into three parts based on its relation to the anterior scalene muscle:
Aneurysms can develop in any of these segments, with varying clinical implications depending on their location.
Subclavian artery aneurysms can arise from several causes, including:
Many subclavian artery aneurysms are asymptomatic and discovered incidentally. When symptoms occur, they may include:
Diagnosis involves a combination of clinical examination and imaging studies:
Treatment depends on the aneurysm’s size, symptoms, and risk of complications.
Indicated for symptomatic aneurysms, large size (>2 cm), or complications such as embolization or rupture risk.
With timely diagnosis and appropriate treatment, the prognosis is generally favorable. Surgical repair has high success rates, and endovascular techniques offer less invasive alternatives with shorter recovery. Untreated aneurysms carry significant risks of rupture and embolic events, which can be fatal.
Seek medical attention if you experience:
Early evaluation by a vascular specialist is essential for diagnosis and management.
Subclavian artery aneurysms, though rare, pose serious health risks due to their potential for rupture and embolization. Understanding the anatomy, causes, and clinical features aids in early detection. Advances in imaging and surgical techniques have improved outcomes significantly. If you suspect any symptoms related to this condition, prompt consultation with a healthcare professional is vital to ensure timely intervention and reduce complications. Maintaining vascular health through lifestyle modifications and regular medical check-ups can also help prevent aneurysm development.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec