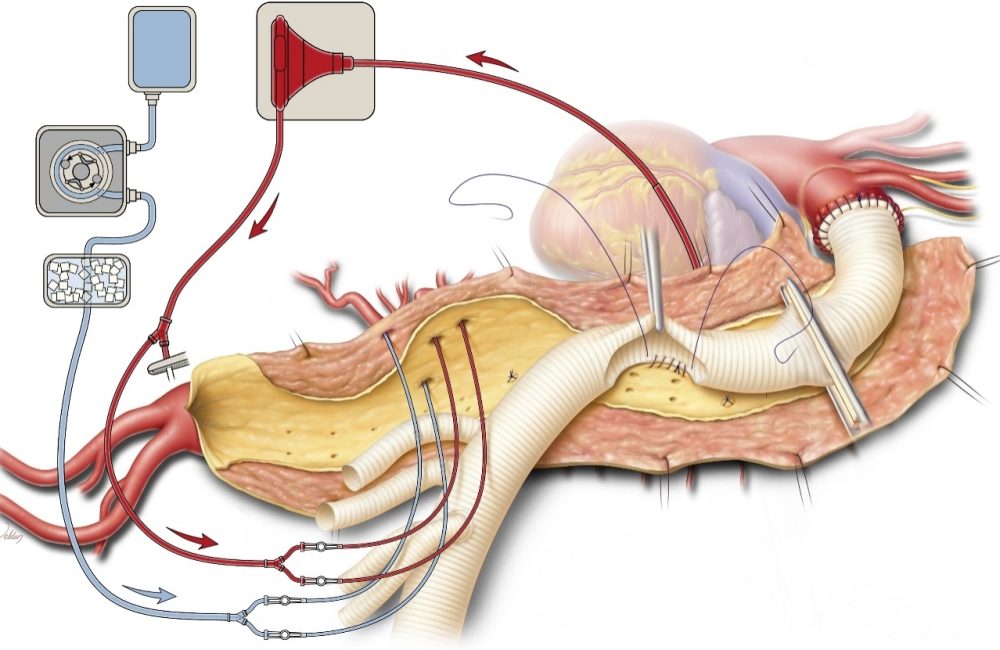
An Arterial Aneurysm is an abnormal, balloon-like bulge in the wall of an artery caused by weakening of its structure. Left untreated, aneurysms can grow, rupture, or form blood clots, leading to life-threatening complications.
Arterial Aneurysm Repair refers to surgical or minimally invasive procedures that reinforce or replace the weakened artery to restore safe blood flow. Repair is often recommended when the aneurysm is large, symptomatic, or at high risk of rupture. The goal is to prevent catastrophic bleeding, preserve circulation, and improve long-term health.
Arteries are blood vessels that carry oxygen-rich blood from the heart to the body. Their walls are made of three layers—intima, media, and adventitia—which provide strength and elasticity.
Common sites of aneurysms include:
Abdominal aorta (Abdominal Aortic Aneurysm, AAA): The most frequent location.
Thoracic aorta: In the chest region.
Peripheral arteries: Such as the popliteal (behind the knee), femoral (in the thigh), or carotid arteries.
An aneurysm develops when part of the arterial wall weakens and bulges outward, similar to a weak spot in a garden hose. The bigger the aneurysm grows, the higher the risk of rupture.
Several factors can contribute to aneurysm formation:
Atherosclerosis: Buildup of fatty deposits that weaken the arterial wall.
High blood pressure (hypertension): Increases wall stress.
Genetic conditions: Such as Marfan syndrome, Ehlers-Danlos syndrome, or familial aneurysm syndromes.
Smoking: Major risk factor for both aneurysm development and rupture.
Age: Risk increases after age 60.
Gender: Males are more commonly affected, though females may face higher rupture risk.
Infection or trauma: Rarely, infections (mycotic aneurysm) or injury can cause localized weakening.
Many aneurysms are silent, discovered only during routine scans. When symptoms occur, they may include:
Abdominal aortic aneurysm (AAA): Pulsating feeling in the abdomen, back pain, abdominal pain.
Thoracic aortic aneurysm: Chest pain, hoarseness, difficulty swallowing, shortness of breath.
Peripheral aneurysm (e.g., popliteal): Swelling behind the knee, leg pain, numbness, or coldness.
Acute rupture: Sudden severe pain, low blood pressure, dizziness, loss of consciousness—this is a medical emergency.
Diagnosis usually involves a combination of clinical examination and imaging tests:
Physical examination: Sometimes a pulsating mass can be felt, especially in abdominal aneurysms.
Ultrasound: Common first-line tool for detecting and measuring aneurysms.
CT angiography (CTA): Provides detailed images of aneurysm size, shape, and relation to other vessels.
MR angiography (MRA): Another option for detailed imaging without radiation.
Plain X-ray: May occasionally show calcification of aneurysm walls.
Management depends on aneurysm size, growth rate, symptoms, and patient health.
Non-surgical management (for small, stable aneurysms):
Regular monitoring with ultrasound or CT scans (“watchful waiting”).
Blood pressure control with medications.
Lifestyle changes—quitting smoking, healthy diet, and regular exercise.
Medications to control cholesterol and reduce vascular risk.
Surgical / procedural management:
Open surgical repair: The diseased artery segment is replaced with a synthetic graft (usually Dacron or PTFE).
Endovascular aneurysm repair (EVAR or TEVAR): A minimally invasive approach where a stent graft is delivered through the arteries (via small groin incisions) and placed inside the aneurysm to reinforce the wall and redirect blood flow.
The choice between open and endovascular repair depends on aneurysm anatomy, patient health, and surgical expertise.
General anesthesia is administered.
An incision is made over the affected artery (e.g., abdomen for AAA).
The aneurysm is carefully opened, and blood flow is temporarily rerouted.
A synthetic graft is sewn into place to replace the weakened artery.
The aneurysm wall is closed over the graft, and the incision is sutured.
Performed under general, regional, or local anesthesia.
Small incisions are made in the groin to access the femoral arteries.
A catheter delivers a stent graft into the aneurysm under X-ray guidance.
The stent expands to line the inside of the artery, sealing off the aneurysm.
Blood flows through the stent graft, reducing pressure on the aneurysm wall.
EVAR generally has a shorter recovery time but requires lifelong surveillance.
Recovery differs between open repair and endovascular repair:
Hospital stay: Typically 7–10 days after open repair, 2–3 days after EVAR.
Pain management and wound care: Critical for healing.
Medications: Antiplatelet agents (e.g., aspirin) and drugs to control blood pressure and cholesterol.
Gradual return to activity: Walking is encouraged early, but heavy lifting is restricted for weeks.
Long-term follow-up:
After open repair: routine check-ups, fewer imaging requirements.
After EVAR: regular CT or ultrasound scans to monitor the stent graft for leaks or movement.
All procedures carry some risks. Potential complications include:
Open repair:
Bleeding
Heart or lung complications
Infection
Kidney problems
Bowel complications
Endovascular repair:
Endoleak (persistent blood flow into aneurysm sac)
Stent migration or blockage
Need for re-intervention
Vascular injury during access
Both approaches aim to prevent rupture, but careful patient selection and follow-up are essential.
Seek medical attention if you experience:
A pulsating sensation in the abdomen.
Unexplained persistent abdominal, chest, or back pain.
Swelling or pain in the leg associated with a known aneurysm.
Sudden severe pain, dizziness, or collapse (call emergency services immediately).
People with risk factors—such as smoking history, high blood pressure, or family history of aneurysm—should ask their doctor about screening.
Arterial Aneurysm Repair is a crucial, often lifesaving procedure that prevents rupture and preserves circulation. Depending on the patient’s condition and aneurysm characteristics, treatment may involve open surgical grafting or minimally invasive endovascular repair.
Regular check-ups, healthy lifestyle choices, and adherence to medical advice play a key role in long-term success. Anyone with risk factors or symptoms of an aneurysm should consult a healthcare professional promptly for evaluation and guidance.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec