Carotid tumours are rare growths that develop in or around the carotid artery, a major blood vessel in the neck responsible for supplying oxygen-rich blood to the brain. These tumours, often referred to as carotid body tumours or paragangliomas, are typically benign but can cause significant health issues due to their location near vital neurovascular structures. Understanding carotid tumours is crucial because early diagnosis and appropriate management can prevent complications such as stroke, nerve damage, or tumour progression. This article provides a detailed overview of carotid tumours, covering anatomy, causes, symptoms, diagnosis, treatment, and prognosis.
The carotid arteries are paired vessels located on each side of the neck. Each artery bifurcates into the internal carotid artery, which supplies blood to the brain, and the external carotid artery, which supplies the face and scalp. At the bifurcation lies the carotid body, a small cluster of chemoreceptor cells that monitor blood oxygen levels and help regulate respiratory activity.
Carotid tumours most commonly arise from the carotid body and are classified as paragangliomas. These tumours originate from paraganglionic tissue, which is part of the autonomic nervous system. Due to their proximity to critical nerves (such as the vagus and hypoglossal nerves) and blood vessels, carotid tumours can affect neurological function and vascular integrity.
The exact cause of carotid tumours is not fully understood, but several factors are associated with their development:
Carotid tumours often grow slowly and may remain asymptomatic for years. When symptoms do appear, they typically include:
Diagnosing carotid tumours involves a combination of clinical examination and imaging studies:
Treatment depends on tumour size, symptoms, patient health, and potential malignancy:
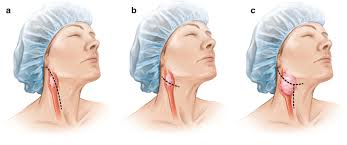
Surgical removal of carotid tumours is a delicate procedure performed by experienced vascular or head and neck surgeons:
Potential risks associated with carotid tumour and its treatment include:
Most carotid tumours are benign and have an excellent prognosis when treated appropriately. Surgical resection offers a high cure rate, especially for localized tumours. Malignant carotid paragangliomas are rare but require more aggressive management and have a variable prognosis. Early diagnosis and treatment significantly improve outcomes and reduce the risk of complications.
Seek medical attention if you notice:
Early evaluation by a healthcare professional can facilitate timely diagnosis and management.
Carotid tumours, though rare, are important vascular lesions that require careful evaluation due to their proximity to critical neurovascular structures. Understanding their anatomy, causes, symptoms, and treatment options is essential for effective management. Surgical resection remains the cornerstone of treatment, with excellent outcomes in most cases. If you experience any suspicious neck masses or related symptoms, consult a healthcare professional promptly to ensure appropriate care and avoid complications.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec