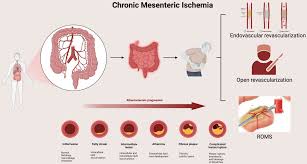
Chronic mesenteric ischemia (CMI) is a rare but serious condition characterized by insufficient blood flow to the intestines due to narrowing or blockage of the mesenteric arteries. The superior mesenteric artery (SMA) and the celiac artery are the primary vessels supplying blood to the gastrointestinal tract. When these arteries become stenosed or occluded, the intestines receive inadequate oxygen and nutrients, leading to symptoms such as abdominal pain and weight loss.
CMI is important because delayed diagnosis and treatment can result in severe complications, including intestinal infarction and malnutrition. Advances in endovascular techniques, such as SMA and celiac artery stenting, have revolutionized treatment by offering minimally invasive options that restore blood flow and improve patient outcomes.
Understanding the anatomy of the mesenteric circulation is essential to grasp the pathophysiology of CMI. The gastrointestinal tract receives blood primarily from three major arteries branching off the abdominal aorta:
The SMA and celiac artery are the most critical vessels in CMI because they supply the majority of the small and upper large intestines. These arteries have collateral connections, but significant stenosis or occlusion can overwhelm compensatory mechanisms, leading to ischemia.
The most common causes and risk factors for chronic mesenteric ischemia include:
Patients with chronic mesenteric ischemia typically present with:
Symptoms are often nonspecific and can mimic other gastrointestinal disorders, which may delay diagnosis.
Diagnosing CMI involves a combination of clinical evaluation and imaging studies:
Endovascular stenting has become the preferred initial treatment due to lower morbidity and faster recovery compared to open surgery.
The stenting procedure typically involves the following steps:
The procedure usually lasts 1–2 hours and may be performed on an outpatient or short-stay basis.
Potential risks and complications of SMA/celiac artery stenting include:
With timely diagnosis and treatment, the prognosis of chronic mesenteric ischemia has improved significantly. Endovascular stenting offers symptom relief in approximately 80–90% of patients, with reduced morbidity compared to open surgery. However, long-term follow-up is essential due to the risk of restenosis. Untreated CMI can lead to life-threatening intestinal infarction and malnutrition.
Seek medical attention if you experience:
Early evaluation by a healthcare professional can prevent complications and improve outcomes.
Chronic mesenteric ischemia is a serious vascular condition caused primarily by atherosclerotic narrowing of the SMA and celiac arteries, leading to intestinal ischemia. Recognizing the characteristic symptoms and obtaining appropriate imaging are critical for diagnosis. Endovascular stenting of the SMA and celiac artery has emerged as a safe and effective treatment, offering symptom relief and improved quality of life. Patients with risk factors or symptoms suggestive of CMI should consult vascular specialists promptly to explore diagnostic and therapeutic options. Early intervention can prevent severe complications and enhance long-term prognosis.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec