Acute mesenteric ischemia (AMI) is a life-threatening condition characterized by a sudden reduction in blood flow to the intestines, leading to ischemia and potential bowel necrosis. Prompt diagnosis and treatment are critical to prevent severe complications and improve survival rates. One of the advanced treatment modalities for AMI caused by arterial thrombosis or embolism in the superior mesenteric artery (SMA) or celiac artery is thrombolysis — a minimally invasive procedure aimed at dissolving the clot and restoring blood flow. This article provides a comprehensive overview of AMI, focusing on thrombolysis of the SMA and celiac artery, highlighting its importance, procedure, and outcomes.
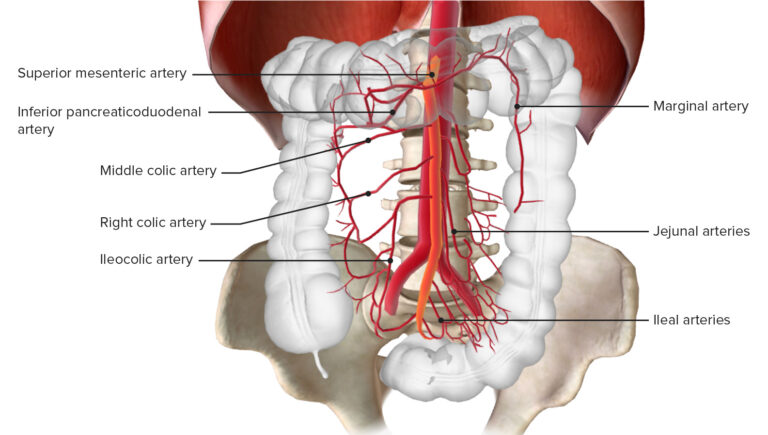
The mesenteric circulation primarily involves the celiac artery, superior mesenteric artery (SMA), and inferior mesenteric artery (IMA), which supply blood to the gastrointestinal tract. The SMA is the most critical vessel for intestinal perfusion, supplying the small intestine, cecum, ascending colon, and part of the transverse colon. The celiac artery supplies the stomach, liver, spleen, and pancreas.
Acute mesenteric ischemia occurs when there is an abrupt interruption of blood flow through these arteries, most commonly the SMA, leading to ischemia of the bowel. The rapid loss of oxygen and nutrients causes mucosal injury, transmural infarction, and if untreated, bowel necrosis and perforation.
The primary causes of acute mesenteric ischemia include:
Risk factors include advanced age, atrial fibrillation, heart failure, atherosclerosis, hypercoagulable states, recent surgery, and hypotension.
Patients with acute mesenteric ischemia typically present with:
Early symptoms can be subtle, making diagnosis challenging.
Diagnosis of AMI involves a combination of clinical suspicion, laboratory tests, and imaging:
Treatment depends on the cause, severity, and timing of diagnosis:
Catheter-directed thrombolysis is a minimally invasive procedure performed by interventional radiologists or vascular surgeons to dissolve thrombi in the SMA or celiac artery.
This procedure can be performed emergently and may avoid the need for open surgery if done early.
Potential risks of thrombolysis include:
The prognosis of AMI depends heavily on the timing of diagnosis and treatment. Early thrombolysis can significantly improve survival by restoring blood flow and preventing bowel infarction. However, mortality rates remain high, ranging from 50% to 70% in untreated or late-treated cases. Prompt intervention and multidisciplinary care are essential for favorable outcomes.
Seek immediate medical attention if you experience:
Early evaluation can be lifesaving.
Acute mesenteric ischemia is a critical vascular emergency requiring high clinical suspicion and rapid intervention. Thrombolysis of the superior mesenteric or celiac artery offers a minimally invasive option to restore intestinal blood flow and reduce the need for extensive surgery. Understanding the anatomy, causes, clinical presentation, and treatment options is vital for timely diagnosis and management. If you or someone you know experiences symptoms suggestive of AMI, immediate consultation with healthcare professionals is imperative to improve outcomes and save lives.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec