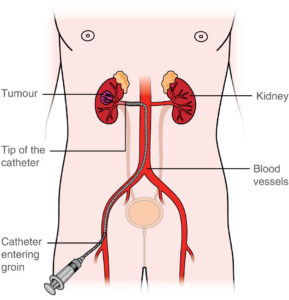
Arterial embolisation is a minimally invasive medical procedure used to deliberately block blood flow in specific arteries. This technique is employed to control bleeding, reduce blood supply to tumors, or manage vascular abnormalities. It plays a crucial role in various clinical settings, including trauma management, oncology, and treatment of vascular malformations. Understanding arterial embolisation is important for patients and healthcare providers alike, as it offers a targeted approach to managing complex vascular conditions with reduced systemic effects compared to traditional surgery.
To appreciate arterial embolisation, it is essential to understand the basic anatomy of the arterial system. Arteries are blood vessels that carry oxygen-rich blood from the heart to tissues throughout the body. They branch into progressively smaller vessels, culminating in capillaries where gas and nutrient exchange occur.
The procedure typically targets specific arteries supplying a pathological area, such as a bleeding site or tumor. For example, embolisation of the uterine arteries is common in treating fibroids, while embolisation of the hepatic artery may be used for liver tumors. The accessibility and branching pattern of arteries influence the approach and success of embolisation.
Arterial embolisation is not a disease but a therapeutic intervention. However, it is used to treat conditions caused by:
Risk factors for conditions requiring embolisation include hypertension, atherosclerosis, trauma, and certain genetic predispositions to vascular anomalies.
Symptoms vary depending on the underlying condition prompting embolisation:
Patients may present acutely in emergency settings or electively for planned procedures.
Diagnosis involves identifying the source of bleeding or the vascular lesion requiring treatment:
Arterial embolisation is a treatment modality itself but is part of a broader management plan:
Arterial embolisation is performed by interventional radiologists under imaging guidance:
The procedure typically lasts 1-3 hours depending on complexity.
After embolisation:
While generally safe, arterial embolisation carries potential risks:
Prompt recognition and management of complications are essential.
The prognosis after arterial embolisation depends on the underlying condition and the success of the procedure:
Seek immediate medical attention if you experience:
For elective procedures, consult your healthcare provider to discuss risks, benefits, and alternatives.
Arterial embolisation is a vital, minimally invasive procedure that effectively manages bleeding, tumors, and vascular abnormalities by selectively occluding arteries. Understanding its indications, procedure, and potential risks empowers patients and clinicians to make informed decisions. If you or a loved one faces conditions that may benefit from embolisation, consult a qualified healthcare professional to explore this treatment option tailored to your needs.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec