Carotid interventions refer to medical and surgical procedures aimed at treating diseases of the carotid arteries, the major blood vessels that supply oxygen-rich blood to the brain. These interventions are crucial in preventing strokes, which can result from carotid artery narrowing or blockage. Stroke is a leading cause of disability and death worldwide, making timely diagnosis and treatment of carotid artery disease essential for preserving neurological function and improving patient outcomes.
The carotid arteries are paired vessels located on each side of the neck. Each carotid artery bifurcates into two branches:
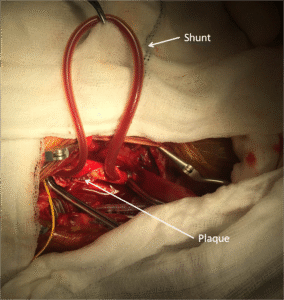
The carotid arteries have three layers: the intima (inner lining), media (muscle layer), and adventitia (outer connective tissue). Atherosclerosis, the buildup of fatty plaques within the intima, is the most common pathological process affecting these arteries, leading to stenosis (narrowing) or occlusion (blockage).
The primary cause of carotid artery disease is atherosclerosis, which develops over years due to the accumulation of cholesterol, inflammatory cells, and fibrous tissue in the arterial walls. Key risk factors include:
Less common causes include carotid artery dissection, fibromuscular dysplasia, radiation-induced injury, and inflammatory conditions such as vasculitis.
Carotid artery disease may be asymptomatic or present with symptoms related to reduced cerebral blood flow or embolism. Common clinical presentations include:
Diagnosis involves a combination of clinical evaluation and imaging studies:
Laboratory tests may assess cardiovascular risk factors such as lipid profile, blood glucose, and inflammatory markers.
Treatment aims to reduce stroke risk by managing atherosclerosis and restoring adequate blood flow.
The choice between CEA and CAS depends on patient-specific factors such as anatomy, comorbidities, and surgical risk.
Potential risks vary by procedure but may include:
With appropriate treatment, the risk of stroke can be significantly reduced. Carotid endarterectomy has demonstrated long-term efficacy in preventing stroke in patients with significant stenosis. Carotid artery stenting offers a less invasive alternative with comparable outcomes in selected patients. Early intervention and strict control of risk factors improve prognosis and quality of life.
Seek medical attention promptly if you experience:
Carotid interventions play a vital role in managing carotid artery disease and preventing stroke. Understanding the anatomy, risk factors, symptoms, and treatment options empowers patients and caregivers to seek appropriate care. Advances in surgical and endovascular techniques have improved safety and outcomes. If you or a loved one experience symptoms suggestive of carotid artery disease, consult a healthcare professional promptly for evaluation and management. Early diagnosis and treatment are key to preserving brain health and preventing debilitating complications.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec