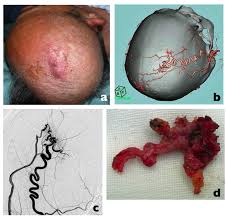
Vascular malformations are abnormal clusters or tangles of blood vessels that can occur anywhere in the body. These congenital anomalies arise from errors in vascular development during embryogenesis and can vary widely in size, location, and clinical impact. Excision of vascular malformations refers to the surgical removal of these abnormal vessels to alleviate symptoms, prevent complications, or improve cosmetic appearance. This procedure is important because untreated vascular malformations can cause pain, bleeding, functional impairment, or disfigurement, significantly affecting a patient’s quality of life.
Understanding the nature of vascular malformations and the role of excision helps patients and caregivers make informed decisions about treatment options. This article provides a detailed, reader-friendly guide on the anatomy, causes, symptoms, diagnosis, treatment, and surgical excision of vascular malformations.
Vascular malformations involve the blood vessels—arteries, veins, capillaries, or lymphatic vessels—that form the circulatory system. Normally, these vessels develop in a highly regulated manner during fetal growth, creating a network that efficiently delivers blood and lymph throughout the body.
Vascular malformations are classified based on the type of vessels involved:
These malformations can be superficial or deep, localized or diffuse, and may infiltrate surrounding tissues, complicating treatment.
Vascular malformations are primarily congenital, resulting from errors in vascular development during embryogenesis. Unlike vascular tumors (e.g., hemangiomas), they do not proliferate but grow proportionally with the individual.
Common causes and risk factors include:
Symptoms depend on the type, size, and location of the vascular malformation. Common clinical features include:
Diagnosing vascular malformations involves a combination of clinical evaluation and imaging studies:
Treatment depends on symptoms, lesion type, size, and patient preference. Options include:
Often, a multidisciplinary approach combining therapies yields the best outcomes.
Potential risks include:
Careful surgical technique and postoperative care minimize these risks.
The prognosis after excision of vascular malformations is generally favorable, especially with complete removal. Many patients experience symptom relief, improved function, and cosmetic enhancement. However, some malformations, particularly extensive or deep lesions, may recur or require additional treatments. Early diagnosis and multidisciplinary management improve outcomes.
Excision of vascular malformations is a critical treatment option for managing these complex vascular anomalies. Understanding the anatomy, causes, symptoms, and treatment modalities empowers patients to make informed decisions. While surgery can be highly effective, it requires careful planning and expert care to minimize risks and optimize outcomes. If you suspect you have a vascular malformation or have been diagnosed with one, consult a qualified healthcare professional to explore the best treatment approach tailored to your needs.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec