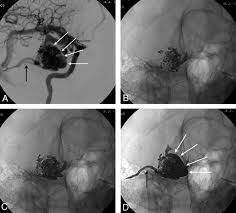
Arteriovenous malformations (AVMs) are abnormal tangles of blood vessels where arteries connect directly to veins without the usual intervening capillaries. This vascular anomaly can disrupt normal blood flow and oxygen circulation, potentially leading to serious complications such as bleeding or neurological deficits. AVM embolization is a minimally invasive procedure designed to block the abnormal blood vessels, reducing the risk of hemorrhage and alleviating symptoms. Understanding AVM embolization is crucial for patients diagnosed with AVMs and healthcare providers managing these complex vascular lesions.
To appreciate AVM embolization, it is important to understand the vascular anatomy involved. Normally, arteries carry oxygen-rich blood from the heart to tissues, branching into smaller arterioles and then capillaries, where oxygen exchange occurs. Blood then flows into venules and veins, returning to the heart.
In an AVM, this capillary network is absent. Instead, arteries connect directly to veins through a nidus — a tangled web of abnormal vessels. This direct connection causes high-pressure arterial blood to flow into veins, which are not designed to handle such pressure, increasing the risk of vessel rupture and bleeding. AVMs can occur anywhere in the body but are most clinically significant when located in the brain or spinal cord.
The exact cause of AVMs is not fully understood, but they are generally considered congenital, meaning they develop during fetal growth. Some key points include:
Many AVMs remain asymptomatic and are discovered incidentally. When symptoms occur, they depend on the AVM’s size and location:
Diagnosing an AVM involves a combination of clinical evaluation and imaging studies:
Treatment depends on the AVM’s size, location, symptoms, and risk of bleeding. Options include:
While embolization is generally safe, potential risks include:
The prognosis after AVM embolization varies:
AVM embolization is a vital, minimally invasive treatment option for managing arteriovenous malformations, particularly in the brain. Understanding the anatomy, symptoms, diagnostic methods, and treatment options empowers patients and caregivers to make informed decisions. While the procedure carries some risks, advances in endovascular techniques have improved safety and outcomes. If you or a loved one has an AVM, consulting with a specialized healthcare professional is essential to determine the best individualized treatment plan and ensure optimal care.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec