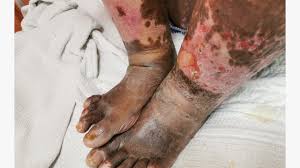
Cellulitis is a common, potentially serious bacterial skin infection that affects the deeper layers of the skin and underlying tissues. It typically presents as a red, swollen, warm, and painful area of skin, often accompanied by fever and malaise. Prompt recognition and treatment of cellulitis are crucial to prevent complications such as abscess formation, sepsis, or the spread of infection to other parts of the body. Understanding cellulitis is important for both healthcare providers and the general public to ensure timely diagnosis and effective management.
The skin is the body’s largest organ and serves as a protective barrier against environmental pathogens. It consists of three main layers:
Epidermis: The outermost layer, providing a waterproof barrier.
Dermis: The middle layer containing connective tissue, blood vessels, and nerves.
Subcutaneous tissue: The deepest layer composed of fat and connective tissue.
Cellulitis involves infection of the dermis and subcutaneous tissues. The infection usually occurs when bacteria enter through a break in the skin, such as a cut, scrape, insect bite, or surgical wound. The most common causative organisms are Streptococcus and Staphylococcus species.
Cellulitis is primarily caused by bacterial invasion of the skin and subcutaneous tissues. Common causes and risk factors include:
Patients with cellulitis typically present with:
Diagnosis of cellulitis is primarily clinical, based on history and physical examination. Key diagnostic steps include:
Surgery is generally not required for uncomplicated cellulitis but may be necessary if:
With prompt and appropriate treatment, cellulitis usually resolves without long-term problems. Most patients recover fully within 7 to 10 days. However, delayed treatment or underlying health issues can lead to complications and prolonged recovery.
Seek medical attention if you experience:
Early evaluation by a healthcare professional is essential to prevent serious complications.
Cellulitis is a common bacterial skin infection that requires timely diagnosis and treatment to avoid complications. Understanding its causes, symptoms, and management options empowers patients and caregivers to seek appropriate care promptly. If you suspect cellulitis, consult a healthcare provider for evaluation and treatment to ensure the best possible outcome.


Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec